A 69-year-old white man was transferred to our hospital with a diagnosis of aneurysm of the ascending aorta and suspected type A acute aortic dissection.
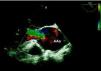
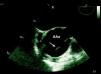
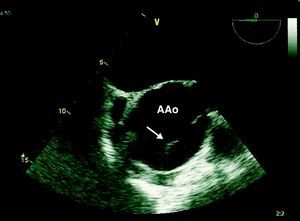
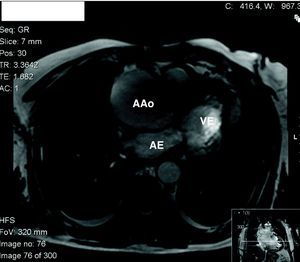
The patient had a history of hypertension, irregularly treated, type 2 diabetes and previous smoking (35 pack/years). He had been experiencing progressively worsening fatigue and exertional dyspnea for a year. The present hospitalization was prompted by thoracic and epigastric pain radiating to the back accompanied by dyspnea, with one day of evolution. Physical observation revealed hypertension and a grade IV/VI aortic diastolic murmur. Initial laboratory tests and electrocardiogram were normal. Transthoracic echocardiography showed marked dilatation of the aortic root and ascending aorta (maximum transverse diameter 71mm) with severe aortic regurgitation. An image suggestive of an intimal flap prompted assessment by transesophageal echocardiography, which confirmed an aneurysmal dilatation of the aortic root and ascending aorta (maximum transverse diameter 71mm) sparing the aortic arch and the descending aorta. The aortic valve was tricuspid and severe regurgitation was seen, due to malcoaptation of the leaflets. A linear image moving relative to the right coronary sinus, suggestive of an intimal flap, was observed, which could have corresponded to the course of a dissection (Figs. 1 and 2). Thoracic computed tomography performed at the original hospital confirmed aortic dilatation but appeared to exclude dissection or rupture.
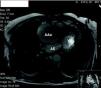
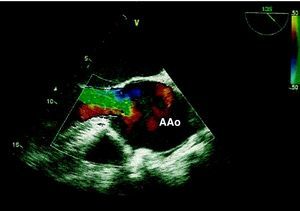
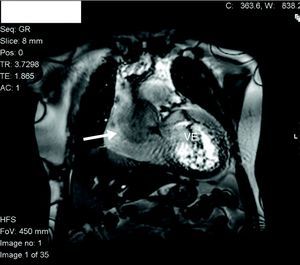
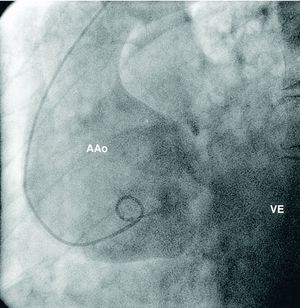
On admission to our hospital the patient was asymptomatic, under therapy with nitrates and beta-blockers and hemodynamically stable. Cardiac magnetic resonance imaging revealed aneurysmal dilatation limited to the aortic root and ascending aorta (maximum transverse diameter 65mm) and excluded dissection or rupture (Figs. 3 and 4). Preoperative cardiac catheterization excluded coronary disease and aortography, performed at the same time, documented annulo-aortic ectasia (maximum transverse diameter of the ascending aorta 75mm) (Fig. 5). The patient underwent a Bentall procedure, a 25-mm Carpentier–Edwards aortic valve and a 28-mm Vascutek tube graft being implanted. The postoperative course was uneventful and the patient was discharged five days later. Anatomopathological analysis of the resected arterial wall showed numerous atherosclerotic plaques with focal ulceration.
Annulo-aortic ectasia can occur in isolation or in the context of generalized connective tissue disease such as Marfan or Ehlers–Danlos syndrome. Most cases of ascending aorta aneurysm are associated with degenerative alterations in the aortic media, unlike most aneurysms of the descending aorta, that are usually due to atherosclerosis. The development of invasive atheromas is associated with extensive destruction of elastic fibers and smooth muscle cells in the media of the aortic wall, which is weakened, predisposing to dilatation.1 Less common causes of annuloaortic ectasia include aneurysms associated with aortic dissection or aortic valve disease (particularly bicuspid aortic valve), aortic arteritis, infection (especially syphilitic), inflammation and trauma.2 The possibility of annulo-aortic ectasia being associated with aortic dissection makes it essential to exclude this diagnosis, but this is often difficult and requires various imaging techniques, as illustrated by the case presented.
Conflicts of interestThe authors have no conflicts of interest to declare.
Please cite this article as: Silva, D. Ectasia anulo-aórtica em imagem. Rev Port Cardiol. 2012. doi:10.1016/j.repc.2012.01.011.