Conduction disturbances requiring permanent pacemaker (PM) implantation occur in 3–12% of patients after aortic valve replacement (AVR). Our aim was to assess long-term PM dependency and its predictors in these patients.
MethodsWe conducted a retrospective study of all consecutive patients undergoing permanent PM implantation after AVR between January 2004 and December 2010. Absence of sinus rhythm or atrial fibrillation with appropriate ventricular response at a pacing rate of 30 bpm for 10 s was defined as pacemaker dependency.
ResultsNinety-one patients underwent permanent PM implantation and during follow-up (1026.6±732.0 days) 64% of them did not recover rhythm. Age, conduction disorders on the preoperative ECG, negative chronotropic medication before surgery, cardiopulmonary bypass and aortic cross-clamp times did not influence rhythm recovery. In multivariate analysis, valvular disease etiology related to endocarditis, prosthetic dysfunction and bicuspid valve were associated with long-term PM dependency (OR 5.05; CI: 1.43–17.75).
ConclusionsThe majority of patients undergoing permanent PM implantation after AVR did not recover from conduction disorders during follow-up. The etiology of valvular disease was an independent predictor of late PM dependence.
Distúrbios da condução que requerem implantação de pacemaker (PM) permanente após a substituição da valva aórtica (SVA) ocorrem em 3-12% dos doentes. O objetivo do estudo foi avaliar a dependência do PM a longo prazo e os seus preditores neste grupo de doentes.
MétodosFoi realizado um estudo retrospetivo de todos os doentes submetidos a implantação de PM definitivo após SVA entre janeiro de 2004 e dezembro de 2010. A ausência de ritmo sinusal ou fibrilação auricular com frequência ventricular adequada sob PM a 30 batimentos/min durante um curto período de 10 segundos foi definido como dependência de PM.
ResultadosNoventa e um pacientes foram submetidos a implantação de PM permanente e durante o período de follow-up (1026,6 ± 732,0 dias) 64% deles não recuperaram o ritmo. A idade, os distúrbios de condução no ECG pré-operatório, uso de medicação cronotrópica negativa antes da cirurgia, o tempo de circulação extracorporal e o tempo de clampagem da aorta não influenciaram a recuperação do ritmo. Na análise multivariada, a etiologia da doença valvular (endocardite, disfunção de prótese ou válvula bicúspide) esteve associada à dependência de PM a longo prazo (OR 5,05; IC: 1,43-17,75).
ConclusõesA maioria dos doentes submetidos a implantação de PM permanente após SVA não recupera dos distúrbios de condução durante o follow-up. A etiologia da doença valvular foi um preditor independente da dependência de PM a longo prazo.
Conduction disturbances requiring permanent pacemaker (PM) implantation occur in 3–12% of patients after surgical aortic valve replacement (AVR).1 There is evidence suggesting that these disturbances may improve over time, but little is known about predictors of that improvement.2–5 Understanding the risk factors for PM dependency may influence the timing of implantation, encouraging early PM implantation in selected patients and avoiding unnecessary implantations in others. The aim of this study was to assess long-term PM dependency and its predictors in patients undergoing AVR.
MethodsWe conducted a retrospective study of all consecutive patients undergoing permanent PM implantation after AVR between January 2004 and December 2010 in our tertiary institution. Patients who underwent associated interventions such as other valve replacement, coronary artery bypass grafting or myectomy were included in the study. Data were obtained from patient files including pacemaker records. Follow-up assessment was defined by the last assessment of the PM. Patients were categorized as pacemaker-dependent or non-dependent. Absence of sinus rhythm or atrial fibrillation with appropriate ventricular response at a pacing rate of 30 bpm for 10 s was defined as pacemaker dependency. Whenever information was not complete, patients were reassessed by a cardiologist specializing in pacing. Patients who had a formal indication for pacemaker implantation before surgery and those who had the device implanted 60 days or more after surgery were excluded.
Differences in demographic and clinical characteristics were compared in two groups of patients, according to the occurrence or not of long-term rhythm recovery, using the chi-square test or Fisher's exact test, as appropriate. A multivariate logistic regression model was fitted to estimate odds ratios (OR) and 95% confidence intervals (CI) in order to estimate the independent effect of baseline characteristics. Two-sided p values of <0.05 were considered statistically significant. The statistical analysis was performed using Stata®, version 11.2 (Stata Corporation, College Station, Texas, USA).
ResultsBetween January 2004 and December 2010, a total of 2254 consecutive patients underwent AVR at our institution. Ninety-one patients, mean age 66±13 years, underwent permanent PM implantation a mean of 10.4±4.7 days after surgery. The leading indication for pacemaker implantation was complete atrioventricular block in 85 patients (93%), followed by slow atrial fibrillation (3%) and other atrioventricular conduction disturbances (3%). The majority of patients underwent more than one surgical procedure; 41% of patients underwent isolated aortic valve replacement (Table 1).
Clinical characteristics of patients undergoing aortic valve replacement (n=91).
| Variable | n (%) |
|---|---|
| Age (years) | 66±13a |
| Male | 49 (54) |
| PM indication | |
| Complete AV block | 85 (93) |
| Slow atrial fibrillation/flutter | 3 (3) |
| Other AV conduction disturbances | 3 (3) |
| Mean time to PM implantation (days) | 10.4±4.7a |
| Isolated AVR | 37 (41) |
| Surgical procedures additional to AVR | |
| Mitral surgery | 15 (16) |
| Tricuspid surgery | 11 (12) |
| CABG | 21 (23) |
| Aortic conduit | 10 (11) |
| Myectomy | 13 (14) |
AV: atrioventricular; AVR: aortic valve replacement; CABG: coronary artery bypass grafting; PM: pacemaker.
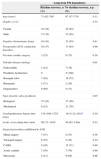
During a mean follow-up of 1026.6±732.0 days, 64% of patients did not recover rhythm. Table 2 shows the incidence of long-term PM dependency according to demographic and clinical variables. Age, gender, negative chronotropic medication before surgery and previous history of cardiac surgery were not associated with long-term PM dependency. Conduction disorders on the preoperative ECG were present in 30% of patients and included first- and second-degree (Mobitz I) AV block and intraventricular block. No association between preoperative conduction disorders and long-term PM dependency was identified.
Long-term pacemaker dependency according to demographic and clinical characteristics.
| Long-term PM dependency | |||
|---|---|---|---|
| Rhythm recovery, n (%) | No rhythm recovery, n (%) | p | |
| Age (years) | 71 (62–78)a | 67 (57–73)a | 0.11 |
| Gender, n (%) | 0.74 | ||
| Female | 16 (38) | 26 (62) | |
| Male | 17 (35) | 32 (65) | |
| Negative chronotropic drugs | 16 (41) | 23 (59) | 0.41 |
| Preoperative ECG conduction disorders | 10 (37) | 17 (63) | 0.96 |
| Previous cardiac surgery | 3 (25) | 9 (75) | 0.38 |
| Valvular disease etiology | 0.01 | ||
| Endocarditis | 2 (22) | 7 (78) | |
| Prosthetic dysfunction | 0 | 5 (100) | |
| Bicuspid valve | 7 (28) | 18 (72) | |
| Rheumatic | 5 (71) | 2 (29) | |
| Degenerative | 9 (69) | 4 (31) | |
| Type of aortic valve prosthesis | 0.07 | ||
| Biological | 27 (42) | 37 (58) | |
| Mechanical | 6 (22) | 21 (78) | |
| Cardiopulmonary bypass time (min) | 134 (108–172)a | 143 (112–201)a | 0.30 |
| Aortic cross-clamp time (min) | 89 (72–118)a | 90 (82–136)a | 0.32 |
| Surgical procedures additional to AVR | |||
| Mitral surgery | 7 (47) | 8 (53) | 0.36 |
| Tricuspid surgery | 6 (55) | 5 (45) | 0.18 |
| CABG | 6 (29) | 15 (71) | 0.40 |
| Aortic conduit | 3 (30) | 7 (70) | 0.66 |
| Myectomy | 4 (31) | 9 (69) | 0.66 |
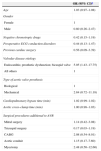
The etiology of valvular disease influenced long-term rhythm recovery (p=0.01). Patients with endocarditis, prosthetic dysfunction or bicuspid valve had a significant risk of no rhythm recovery (OR 2.86; 95% CI 1.14–7.19) compared to other patients (rheumatic, degenerative or unknown etiology). The risk of no rhythm recovery was higher in patients who received a mechanical compared to a biological valve (78% vs. 58%, p=0.07). Cardiopulmonary bypass, aortic cross-clamp times and surgical procedures additional to AVR did not influence rhythm recovery. In multivariate analysis (adjusted for all study variables), valvular disease etiology (including endocarditis, prosthetic dysfunction or bicuspid valve) was the only independent predictor of long-term PM dependency, with a five-fold increase in no rhythm recovery (Table 3). The time to PM implantation was similar between patients with and without rhythm recovery (11.0±4.9 days after surgery vs. 10.1±4.6 days after surgery, respectively; p=0.39), and thus did not influence the probability of rhythm recovery.
Predictors of rhythm recovery.
| OR (95% CI)a | |
|---|---|
| Age | 1.03 (0.97–1.08) |
| Gender | |
| Female | 1 |
| Male | 0.80 (0.26–2.47) |
| Negative chronotropic drugs | 0.42 (0.15–1.19) |
| Preoperative ECG conduction disorders | 0.44 (0.13–1.47) |
| Previous cardiac surgery | 0.56 (0.09–3.39) |
| Valvular disease etiology | |
| Endocarditis; prosthetic dysfunction; bicuspid valve | 5.05 (1.43–17.75) |
| All others | 1 |
| Type of aortic valve prosthesis | |
| Biological | 1 |
| Mechanical | 2.84 (0.72–11.18) |
| Cardiopulmonary bypass time (min) | 1.02 (0.99–1.02) |
| Aortic cross–clamp time (min) | 1.00 (0.98–1.03) |
| Surgical procedures additional to AVR | |
| Mitral surgery | 1.14 (0.42–3.08) |
| Tricuspid surgery | 0.17 (0.03–1.19) |
| CABG | 2.08 (0.54–8.01) |
| Aortic conduit | 1.15 (0.17–7.60) |
| Myectomy | 2.48 (0.50–12.60) |
AVR: aortic valve replacement; CABG: coronary artery bypass grafting; CI: confidence interval; OR: odds ratio.
In the present study we observed a rate of 4% permanent pacemaker implantation following AVR, on the low side of the described rate of 3–12%.1
The few studies to analyze long-term PM dependency show conflicting results with respect to dependency rate and its predictors, as well as with respect to the definition of dependency. Glikson et al.5 reported a heart rhythm recovery rate of 41% after cardiac surgery. Status was defined as non-dependent if patient records showed sinus rhythm or atrial fibrillation with appropriate ventricular response at down-regulation of pacing frequency to the lowest programmable rate for 15 min. Only complete atrioventricular block was significantly associated with long-term PM dependency. Merin et al.4 also analyzed patients undergoing different cardiac surgical procedures; 63% remained PM dependent after a mean follow-up of 72 months. In this study PM dependency was defined by pacing activity when the pacing rate was lowered to 40 bpm for 10 s. In multivariate analysis, preoperative left bundle branch block and third-degree AV block were predictors for late PM dependency. Huynh et al.6 studied a cohort undergoing AVR, of whom 70% were PM dependent after a mean of 32 months. PM dependency was defined as absence of escape rhythm at a pacing rate of 30 bpm for 30 s. Onalan et al.3 defined PM dependency as any PM activity with a pacing rate of 30 bpm, reporting 49% long-term recovery in an AVR cohort. Preoperative history of syncope, bypass time ≥105 min and atrioventricular block as PM indication were independent predictors of long-term PM dependency. Baraki et al.7 included patients with isolated AVR, only 9% of whom recovered rhythm in a mean follow-up of five years. In this case the definition of non-dependency required no pacemaker activity during the previous six months. They did not identify any relation between pre- or perioperative parameters and long-term PM dependency. On the other hand, Raza et al.2 concluded that the majority (60%) of patients who required a PM after cardiac surgery were not dependent during a mean follow-up of six years. PM dependence was determined by reducing the pacing rate to 40 bpm for 30 s. Those who were 100% paced at this rate were classified as PM dependent. In multivariate analysis, a PR interval >200 ms was independently associated with late dependency. These conflicting results may be related to differences in study populations and definitions of PM dependency; studies with a more permissive dependency definition, like that of Raza et al.,2 showed a higher rhythm recovery. Our definition was close to that of Merin et al.4 and Huynh et al.,6 and presents a similar late dependency PM rate.
Few predictors of long-term PM dependency are identified in these studies2–7 and there is little agreement. In most, preoperative conduction disorders were not associated with PM dependency, as confirmed in our cohort. On the other hand, our results highlight the importance of valvular disease etiology. Endocarditis, prosthetic dysfunction and bicuspid valve were independently associated with late PM dependency. Aortic valve endocarditis by itself can cause severe conduction defects. Extensive and aggressive debridement or injury of annular tissue and surrounding structures may cause direct trauma of the conduction system during AVR for endocarditis or redo AVR for prosthetic dysfunction. In bicuspid aortic valve, extensive calcification and aortic root replacement may be the underlying mechanism. Nevertheless a primary conduction system disorder, similar to that seen in other connective tissue disorders, may be responsible and requires further investigation.8
In view of these results we believe that time to PM implantation can be improved in this population. Although current European Society of Cardiology guidelines recommend a period of seven days of persistent AV block postsurgery prior to PM implantation, we suggest that in cases of endocarditis, prosthetic dysfunction and calcified bicuspid valve permanent PM implantation could be performed earlier.
Certain limitations of our study must be acknowledged. Assessment of PM dependency in the short term can underestimate dependency. Non-dependent status in the long term does not mean that PM implantation was unnecessary. We do not know whether these patients are intermittently PM dependent.
ConclusionsThe majority of patients undergoing permanent PM implantation after AVR remain PM-dependent during long-term follow-up. The etiology of valvular disease was an independent predictor of no rhythm recovery in follow-up; patients with endocarditis, prosthetic dysfunction or bicuspid valve had significantly greater PM dependency. In these patients permanent PM implantation may be performed earlier, leading to decreases in immobility and hospitalization.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of interestThe authors have no conflicts of interest to declare.
We thank Aurora Andrade for her expert assistance in data acquisition.