Mitral annulus calcification is a common echocardiographic finding, particularly in the elderly and in end-stage renal disease patients under chronic dialysis. Caseous calcification or liquefaction necrosis of mitral annulus calcification is a rare evolution of mitral annular calcification. Early recognition of this entity avoids an invasive diagnostic approach, since it is benign and, unlike intracardiac tumors and abscesses, has a favorable prognosis. The authors present the case of an 84-year-old woman with a suspicious large, echodense mass at the level of the posterior mitral leaflet with associated severe mitral regurgitation. Cardiac magnetic resonance imaging demonstrated a hypoperfused mass with strong peripheral enhancement 10 minutes after gadolinium administration. Multislice computed tomography showed the calcified nature of the mass. A multi-modality imaging approach confirmed the diagnosis of caseous calcification of the posterior mitral annulus. The patient refused surgical treatment.
A calcificação do anel mitral é um achado ecocardiográfico comum, particularmente em idosos e doentes com insuficiência renal terminal em diálise. A degenerescêncica caseosa, ou necrose liquefeita, da calcificação do anel mitral é uma forma rara de calcificação do anel mitral. O reconhecimento precoce desta entidade evita procedimentos diagnósticos invasivos na medida em que é uma patologia benigna e, ao contrário de tumores e abcesso cardíacos, tem um bom prognóstico. Os autores apresentam o caso clínico de uma doente de 84 anos de idade com uma massa hiperecogénica ao nível do folheto posterior da válvula mitral, associada a insuficiência mitral severa. A ressonância magnética cardíaca demonstrou uma massa hipoperfundida, com realce tardio, após administração de gadolíneo. A tomografia computadorizada cardíaca evidenciou a natureza calcificada da lesão. Uma abordagem multi-imagem permitiu o diagnóstico de calcificação caseosa do anel mitral posterior. A doente recusou cirurgia cardíaca.
Mitral annulus calcification is a common echocardiographic finding, particularly in the elderly and in end-stage renal disease patients under chronic dialysis.1 Caseous calcification of the mitral annulus (CCMA) or liquefaction necrosis of mitral annulus calcification is a rare evolution of mitral annular calcification, with a prevalence of 0.6% in this population and of 0.06–0.07% in large series of patients of all ages.2,3 Early recognition of this entity avoids an invasive diagnostic approach, since it is benign and, unlike intracardiac tumors and abscesses, has a favorable prognosis.2–4,8–10 Echocardiography typically identifies this entity as a round, calcified mass with an echolucent, liquid-like inner part. The authors present the case of an 84-year-old woman with caseous calcification of the posterior mitral annulus.
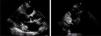
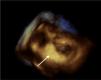
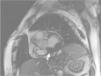
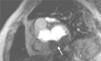
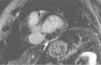
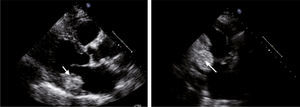
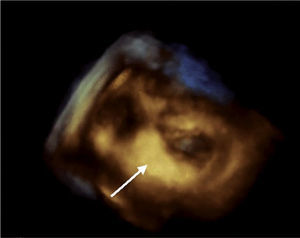
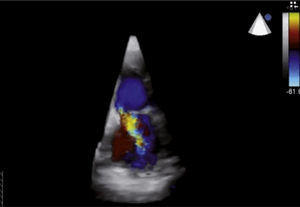
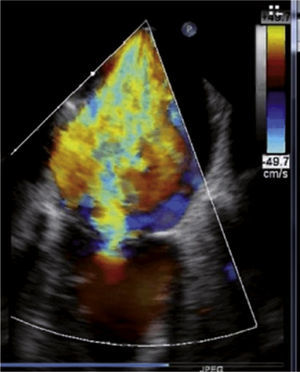
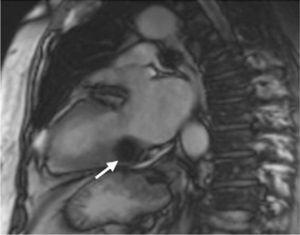
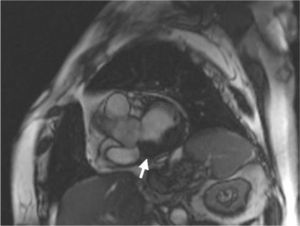
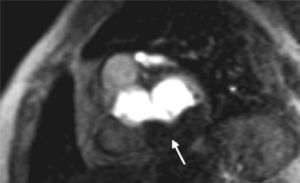
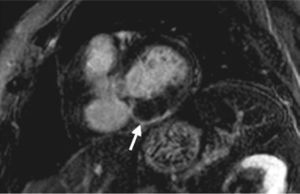
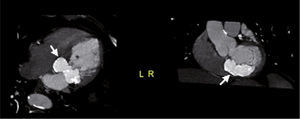
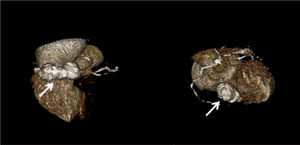
Case reportAn 84-year-old woman, with a history of hypertension and dyslipidemia, was admitted to our institution because of an intracardiac mass. She described a five-month history of shortness of breath on exertion (NYHA functional class III) and peripheral edema. Physical examination revealed a grade III/VI mitral systolic murmur. The electrocardiogram was unremarkable. Laboratory tests results showed no significant alterations. The transthoracic echocardiogram demonstrated a large, round, heterogeneous, echodense mass at the base of the posterior leaflet (Fig. 1). Doppler examination documented severe mitral regurgitation. The three-dimensional transthoracic echocardiogram revealed the mass involving the posterior mitral annulus, distorting it into a more triangular shape (Fig. 2). Three-dimensional transthoracic color flow imaging showed an eccentric mitral regurgitation jet originating from the posteromedial commissure (Fig. 3). The transesophageal echocardiogram confirmed the location of the mass and severe mitral regurgitation (Fig. 4), with two jets identified, one central and the other eccentric, apparently originating from the posteromedial commissure. Cardiac magnetic resonance (CMR) imaging was performed to better evaluate the mass. This showed a hypointense mass in the posterior region of the mitral annulus/basal segment of the inferior wall (Figs. 5 and 6). Rest perfusion CMR demonstrated hypoperfusion of the mass compared to normal myocardium (Fig. 7). Phase-sensitive inversion-recovery CMR showed late gadolinium enhancement in the peripheral margin of the mass (Fig. 8). On the basis of the above findings, a presumptive diagnosis of a centrally liquefied mass containing a high-protein or hemorrhagic content with an inflammatory and/or fibrotic wall was made. A multislice computed tomography (CT) scan of the heart was also performed, demonstrating a relatively homogeneous, high-density mass with foci of calcification (Figs. 9 and 10). A multi-modality imaging approach confirmed the diagnosis of caseous calcification of the posterior mitral annulus.
The patient refused surgery. Medical treatment was optimized.
DiscussionCCMA is a rare evolution of mitral annular calcification.2,3 Echocardiography typically identifies this entity as a round, calcified, echogenic mass.4 CMR reveals a mass between the posterior mitral annulus and adjacent myocardium, with no enhancement after contrast administration and with strong peripheral enhancement 10 minutes after gadolinium administration with the use of the contrast-enhanced inversion-recovery technique.5 CT confirms the calcified aspect of the mass. Histological examination of the inner fluid usually reveals an amorphous, basophilic content, composed of a putty-like admixture of fatty acids, cholesterol, calcium and inflammatory cells, mainly macrophages.4,6 Early recognition of this entity avoids an invasive diagnostic approach, since it is benign and, unlike intracardiac tumors and abscesses, has a favorable prognosis.7 Surgery should be reserved for cases with severe co-existent mitral valve dysfunction, originating from compromised mitral leaflet coaptation secondary to mitral annulus distortion due to CCMA. There are brief references in the literature to possible spontaneous resolution of this entity.8,9 CCMA may rarely be associated with heart rhythm disturbances and systemic embolism.10
ConclusionsCaseous calcification of the mitral annulus (CCMA) or liquefaction necrosis of mitral annulus calcification is a rare evolution of mitral annular calcification. Although transthoracic echocardiography can be sensitive in diagnosing this entity, the diagnosis can sometimes still be inconclusive. Multi-modality imaging with CMR or CT can lead to a definitive diagnosis, avoiding a surgical approach. Once the diagnosis is made, the patient should be treated medically and be monitored clinically and echocardiographically unless there is associated severe mitral valve dysfunction, in which case cardiac surgery is the best therapeutic option.
Conflicts of interestThe authors have no conflicts of interest to declare.