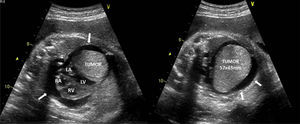
The authors report the case of a 29-year-old woman with an uneventful pregnancy until 35 weeks of gestational age, when a single fetal giant cardiac mass and moderate pericardial effusion were detected on a routine fetal obstetric scan. The mass measured 57 mm×43 mm and was adjacent to the anterior and lateral walls of the left ventricle, causing mild compression, with no signs of inflow or outflow tract obstruction (Figure 1, Videos 1-3). Global cardiac function was preserved and no signs of hemodynamic compromise were documented. All findings were considered consistent with a single cardiac rhabdomyoma.
Fetal echocardiogram at 35 weeks of gestation (4-chamber view): single cardiac mass adjacent to the left ventricle (57 mm×43 mm), with well-defined contours and homogeneous echogenicity, mild left ventricular compression and moderate pericardial effusion (arrows). LA: left atrium; LV: left ventricle; RA: right atrium; RV: right ventricle.
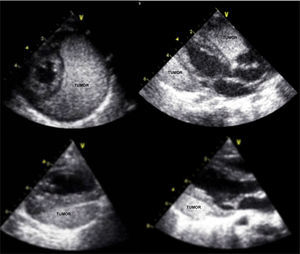
Considering the risk of hemodynamic compromise and interference with lung development, a multidisciplinary decision was made to deliver at 36 weeks by cesarean section. The patient was born in good condition and no hemodynamic compromise or other organ lesions were ever documented. A conservative approach was taken and the patient remained completely asymptomatic, clinically stable under diuretic therapy, gaining weight, with significant regression of pericardial effusion and tumor dimensions documented over time (Figure 2).
Despite the tumor's massive size and location, almost as large as the whole heart and adjacent to the left ventricle, the clinical course was excellent, with documented tumor reduction and no need for intervention.
When established, antenatal diagnosis enables a focused specialized and multidisciplinary approach with individual case management, potentially reducing perinatal morbidity and mortality.
Ethical disclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of interestThe authors have no conflicts of interest to declare.
Videos 1-3 Very well-delimited single fetal giant cardiac mass with homogenous echogenicity, adjacent to the anterior and lateral walls of the left ventricle, measuring 57 mm×43 mm, with moderate to severe pericardial effusion. No inflow or outflow tract obstruction is seen and global cardiac function is preserved.