Myocarditis has spontaneous resolution in 50% of patients. Our study aimed to define risk factors for developing dilated cardiomyopathy (DCM) and death in pediatric patients with acute myocarditis (AM).
MethodsThe retrospective cohort study included all patients with treated AM. The Mother and Child Health Institute from January 2011 to March 2019.
ResultsIn the study, 62 patients were included, 40 boys and 22 girls (11.15±5.86 years) with AM. Twelve out of sixty-two children had acute fulminant myocarditis. Four patients died in the acute phase of AM, and 11 developed DCM. Follow up was 27.14±36.52 months. Patients with poor outcome (DCM development) were under the age of seven (odds ratio [OR] 10.1; p=0.003), more likely to be girls (OR 4.6; p=0.03), and had fulminant myocarditis (OR 27.0; <0.001). An ejection fraction (EF) <55% and fractional shortening (FS) <30% increased risk of DCM 13- and 5-fold, respectively, but patients with EF between 40 and 55% remain at highest risk of developing DCM. There was a 12-fold increased risk for DCM in patients with left ventricular end-diastolic diameter Z score >2+. The receiver operator curve showed that the lactate dehydrogenase (LDH) cut-off value for developing DCM was 1780 mmol/l (sensitivity 80%, specificity 100%).
ConclusionAcute fulminant myocarditis was an independent risk factor for DCM. Children with EF between 40 and 50% at admission were at highest risk of developing DCM. Lactate dehydrogenase value could be a significant prognostic value for the outcome of pediatric myocarditis.
A miocardite tem resolução espontânea em 50% dos doentes. O nosso estudo teve como objetivo definir os fatores de risco para o desenvolvimento de miocardiopatia dilatada (MCD) e de morte em doentes pediátricos com miocardite aguda (MA).
MétodosEstudo de coorte, retrospetivo, que incluiu todos os doentes com MA tratados no The Mother and Child Health Institute entre janeiro de 2011 e março de 2019.
ResultadosForam incluídos 62 doentes, 40 do sexo masculino e 22 do feminino (11,15±5,86 anos) com MA. Das 62 crianças, 12 tiveram MA fulminante. Quatro doentes morreram na fase aguda da MA e 11 desenvolveram MCD. O seguimento decorreu durante 27,14±36,52 meses. Os doentes com prognóstico adverso (desenvolvimento de MCD) tinham menos de sete anos (OR 10,1; p=0,003), eram mais frequentemente do sexo feminino (OR 4,6; p=0,03) e tiveram miocardite fulminante (OR 27,0; <0,001). Uma fração de ejeção <55% e uma fração de encurtamento <30% aumentaram o risco de MCD 13 e 5 vezes, respetivamente, mas os doentes com FE entre 40-55% foram os que tiveram maior risco de desenvolver MCD. O risco de MCD foi 12 vezes superior nos doentes com Z score do diâmetro diastólico do VE maior do que 2+. A curva ROC mostrou que os valores cut-off de desidrogenase láctica (LDH) para o desenvolvimento de MCD foram de 1.780 mmol/l (sensibilidade 80%, especificidade 100%).
ConclusãoA miocardite aguda fulminante foi um fator de risco independente para evolução para MCD. As crianças com FE entre 40-55% na admissão apresentaram o risco mais elevado de desenvolver MCD. O valor da LDH pode ser um fator prognóstico na miocardite pediátrica.
Myocarditis is a significant cause of morbidity and mortality in children despite its low prevalence.1,2 It is estimated to occur in about 0.05% of children, however the existence of asymptomatic patients should be considered due to the lack of accurate data on incidence.3,4 Viruses are the most common etiological factor. Although in most the cases, spontaneous repair after acute myocarditis (AM) was observed, approximately 20% of AM cases lead to chronic myocarditis, dilated cardiomyopathy (DCM) or sudden cardiac death. The development of DCM progresses through three stages: In the acute phase, infection induces cardiomyocyte damage; in the subacute phase, the innate immune response remains activated due to presentation of its own previously unrepresented antigens and molecular mimicry, and leads to myocardial injury; in the chronic phase, inflammation progresses, fibroblasts start to proliferate and differentiate into myofibroblasts to replace the lost cardiomyocytes, which leads to ventricular repair, remodeling, and DCM, an irreversible disease with systolic and diastolic dysfunction.5
Inflammatory myocardial injury is the cause of 27-30% of DCM and of more than 80% of heart transplantations in the pediatric age, with the exception of patients with congenital heart diseases.1 Additionally, prospective postmortem studies concluded that myocarditis was the cause of death in 8.6-12% of young, healthy individuals.6
Our study aimed to establish the risk factors that affect poor prognosis of AM in a pediatric population.
Material and methodsA retrospective cohort study included children under the age of 18 with a diagnosis of AM treated at The Mother and Child Health Institute of Serbia “Dr. Vukan Cupic” from January 2011 to March 2019. The diagnosis of myocarditis was made based on the criteria of the European Society of Cardiology (ESC).7 According to ESC recommendations, at least one symptom (chest pain, palpitations, fatigue, dyspnea, signs of cardiogenic shock) and at least one of the following diagnostic criteria are required to confirm the diagnosis: 1) raised cardiac-specific enzymes (cardiac troponin I [cTnI], and T [cTnT]); 2) abnormalities on electrocardiogram (ECG); 3) functional and structural abnormalities determined by echocardiography and cardiac magnetic resonance imaging (CMR); and 4) tissue characterization by CMR. In asymptomatic patients, at least two diagnostic criteria are required.7 Acute fulminant myocarditis (AFM) is a peculiar clinical condition. It is an acute form of myocarditis, whose main characteristic is a rapidly progressive clinical course due to a sudden and severe inflammation of the myocardium resulting in myocyte necrosis, edema, and cardiogenic shock with the need for hemodynamic, inotropic and respiratory support.8
At our clinic, endomyocardial biopsy (EMB) is not routinely performed, but in all patients polymerase chain reaction (PCR) for the detection of cardiotropic viral nucleic acid in the blood, pericardial fluid, pharyngeal swab, and stool tests were performed. The nucleic acid of the following viruses was examined: adenoviruses, coxsackieviruses, cytomegalovirus (CMV), Epstein-Barr virus (EBV), parvovirus B19, herpes simplex virus (HSV), and influenza. Based on the PCR, all patients were divided into two groups: PCR positive and PCR negative myocarditis.
Newly abnormal ECG included: I to III-degree atrioventricular block or bundle branch block, ST/T wave changes, sinus arrest, ventricular tachycardia or fibrillation, supraventricular tachycardia or atrial fibrillation and frequent premature beats.
Patients with AFM required intubation with mechanical respiratory and hemodynamic support plus vasopressors, inotropes, intravenous diuretics, and intravenous immunoglobulin (IVIG). Hemodynamically unstable patients with AM were treated with inotropes and intravenous diuretics in the intensive care unit. Hemodynamically stable patients were treated with standard heart failure (HF) therapy, including angiotensin-converting enzyme inhibitors, diuretics (spironolactone and furosemide), and β-blockers (carvedilol). Instead in AMF, IVIG was administered in patients with both progressive clinical course and signs of heart failure (HF) (EF<50%, FS 25%, and/or end-diastolic diameter (EDD) Z score >2+). Antiarrhythmics were administered in patients with ventricular arrhythmias.
The impact of demographic characteristics, clinical presentation, ECG, laboratory, echocardiographic parameters, and therapy on the disease outcome were retrospectively analyzed. Patients were compared according to the disease outcome – positive and adverse. Adverse disease outcomes were defined as death and DCM development. Dilated cardiomyopathy was a clinical diagnosis characterized by dilation and impaired contraction of the left or both ventricles, in the absence of coronary artery disease and abnormal loading conditions, which continue after the normalization of the AM parameters.
The follow-up period covered the time elapsed from the end of the acute phase of myocarditis to the last check up at the Institute's cardiology outpatient unit.
Descriptive statistics included mean values, standard deviation, median, and interquartile range of monitored parameters. The difference in the distribution of specific parameters among the groups under test was determined using the chi-square or Fisher's test. The normality of the distribution of numerical variables was tested using the Shapiro Wilk and Kolmogorov Smirnov tests. The comparisons were made between the groups using the Student T-test, ANOVA, Mann Whitney test, and Kruskal Wallis test. Binominal and multinomial logistic regression analyses were used to explain the relationship between the dependent binary variable and independent variables. Cut-off values for enzymes in DCM were defined by receiver operating characteristic (ROC) curve. All statistical methods were significant if p≤0.05. Data processing was performed using statistical software SPSS 25.0 for Windows 10.
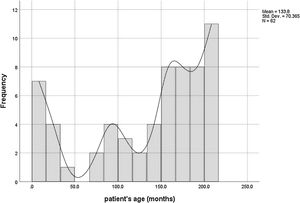
ResultsThe retrospective cohort study included 62 patients, 40 boys and 22 girls, with an average age of 11.15±5.86 years. The occurrence of AM in our patients showed a trimodal distribution concerning age (Figure 1). Polymerase chain reaction positive myocarditis accounted for 30.6% of patients (19/62). The most common isolated virus was CMV (6/19), followed by coxsackievirus (5/19), adenovirus (4/19), parvovirus B19 (2/19), EBV, and HSV. Acute fulminant myocarditis was reported in 12/62 (19.4%) patients, more frequently in younger children (6.9±7.9 vs. 12.6±4.8 years; p=0.0005). All of them required mechanical respiratory support (12/62). Inotropic support was needed by 20/62 patients. Concomitant pericardial affection was observed in 40.3% of patients. Dilated cardiomyopathy developed in 11/60 patients, while a fatal outcome was reported in four patients (5.3%).
Chest pain was the most common symptom (30/62), followed by fever (28/60; average 38.77±0.84°C) and tachycardia (22/62; mean 111.35±33.36/minute). Of 54/62 symptomatic patients, 24/54 had two diagnostic criteria for AM (Table 1). The median number of diagnostic criteria in symptomatic patients was 2 (interquartile range [IQR] 1-2), and in asymptomatic 3 (IQR 2-3). None of the patients with chest pain had an adverse outcome (0/29; p<0.001). This group included all patients with pericarditis. There was a 46-fold increase in risk of an adverse outcome in children with signs and symptoms of HF (8/62) (OR 46.67, 95% CI 4.85-449.086; p<0.001).
Diagnostic criteria for clinically suspected myocarditis according ESC guidelines.7
| Positive diagnostic criteria (number) | Symptoms | |
|---|---|---|
| yes | no | |
| 1 | 18 | - |
| 2 | 24 | 3 |
| 3 | 12 | 5 |
| Total number of patients | 54 | 8 |
Electrocardiogram abnormalities were reported in 33/62 patients, most commonly in the form of ST-segment elevation, and negative T waves in precordial leads, respectively. One patient had ventricular tachycardia upon admission; sinus tachycardia was recorded in 22 patients.
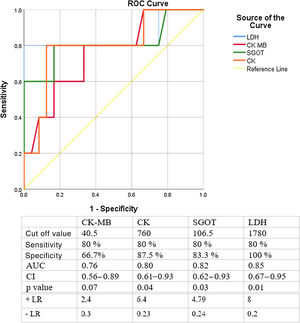
The average values of serum cardiac-specific enzymes at admission are shown in Table 2. These enzymes were measured between day 2 and day 4 after symptom onset. Creatine kinase (CK), creatine kinase (CK) isoform muscle brain (CK-MB), lactate dehydrogenase (LDH), aspartate (SGOT) and alanine aminotransferases (SGPT) were significantly higher in the group of patients with a poor outcome (DCM) than in the group with a favorable outcome (Table 1). Forty-three out of sixty-two children had an increased level of cTnT and cTnI. The average values for cTnI and cTnT were 8.1±8.8 and 2.14±2.95 ng/ml, respectively, but no difference was observed between groups. Patients with AFM had a lower C reactive protein (CRP) serum value than those with AM (10.06±15.1 vs. 91.2±80.6 mg/l; p=0.012). In comparison to children with AM, patients with AFM had higher serum values of CK-MB (p=0.003), SGOT (p=0.018), and LDH (p=0.004). The ROC curve showed that the LDH cutoff values for the development of DCM were 1780 mmol/l (sensitivity 80%, specificity 100%) (Figure 2).
Difference between cardio specific enzymes in two groups of patients – with adverse and unfavorable outcome.
| Enzymes | All patients | Favourable | DCM | p value |
|---|---|---|---|---|
| CK (IJ/l) | 1686.6±7697.2 | 499.2±495.9 | 579.13±1870.6 | 0.02 |
| CK – MB (IJ/l) | 79.1±112.6 | 56.6±60.4 | 147.14±223.2 | 0.05 |
| LDH (IJ/l) | 1375.5±2517.1 | 787.3±609.1 | 3309.3±5227.3 | 0.006 |
| SGPT (IJ/l) | 154.9±455.3 | 51.8±68.8 | 581.2±977.7 | <0.001 |
| SGOT (IJ/l) | 233.3±731.2 | 71.6±80.7 | 819.7±1591.1 | 0.003 |
| cTnT (ng/ml) | 2.14±2.95 | 2.34±3.22 | 1.33±1.15 | 0.60 |
| cTnI (ng/ml) | 8.1±8.8 | 7.9±8.8 | 6.55±8.81 | 0.75 |
Legend: CK-MB: creatine kinase isoform muscle-brain; cTnT: Troponin T; cTnI: Troponin I; DCM: dilated cardiomyopathy LDH: lactate dehydrogenase; SGOT: serum aspartate aminotransferase; SGPT: serum alanine aminotransferase.
Laboratory cutoff values for DCM development - ROC curve. Legend: AUC: area under the curve; CI: confidence interval; CK: creatine kinase; CK-MB: Creatine kinase isoform muscle-brain; LDH: lactate dehydrogenase; + LR: positive likelihood ratio; - LR: negative likelihood ratio; SGOT: serum glutamic oxaloacetic transaminase.
Cardiac magnetic resonance was performed in 14/62 patients in the last 3 years of our study. In 10/14 children, myocardial edema on the T2-weighted sequence was described, while 8/10 had positive late gadolinium enhancement. Average left ventricular ejection fraction (LVEF) was 56.4±15.2%, and normalized left ventricular (LV) end-diastolic volume was 102.8±29.9 ml/m2.
Patients with poor outcome (DCM development) were under the age of seven, were more likely to be girls, and had fulminant myocarditis (Table 3). Patients who developed DCM had a significantly lower EF (42.5±16.1 vs. 58.0±11.0%; p<0.001), FS (21.9±10.9 vs. 33.3±7.3%; p<0.001), and higher LV EDD Z score in comparison to the patients with positive outcome (p<0.001). Patients with EF <55% (26/62), FS <30% (20/62), and LV EDD Z score >2+ (12/62) had a 5, 13, and 12-fold increased risk of DCM, respectively (EF OR 5, 95% confidence interval [CI] 1.8-16.4; p=0.002, FS OR 12, 95% CI 2.470.9; p=0.003, LV EDD Z score >2+ OR 12, 95% CI 2.2-66.3; p=0.004). Abnormal regional wall motions were observed in 16/62 patients. According to the univariate regression analysis, the risk of DCM rose three times with each increase of one in the LV EDD Z score. Patients with PCR-positive myocarditis were at three times an increased risk for some adverse outcome (OR 3.3, 95% CI 0.9-11.1). AFM was an independent risk factor for DCM (Table 4).
Risk factors for dilated cardiomyopathy developing in patients with acute myocarditis – univariate analysis.
| Number of patients | p value | OR | 95% CI | |
|---|---|---|---|---|
| Female gender | 22 | 0.03 | 4.6 | 1.4-18.3 |
| Under the age of 7 years | 14 | 0.003 | 10.1 | 2.23-45.45 |
| Fulminant | 12 | <0.001 | 27.0 | 4.25-171.3 |
| EF<55% | 26 | 0.002 | 5.5 | 1.8-16.4 |
| FS<30% | 20 | 0.003 | 13.1 | 2.4-070.9 |
| LV EDD (z score) | 62 | 0.002 | 3.2 | 1.5-6.8 |
Legend: CI: confidence interval; DCM: dilated cardiomyopathy; EDD: end-diastolic diameter; EF: ejection fraction; FS: fractional shortening; LV: left ventricular; OR: Odds ratio.
Multinomial regression analysis – risk factors for dilated cardiomyopathy.
| Number of patients | p value | OR | 95% CI | |
|---|---|---|---|---|
| PCR positive | 19 | 0.6 | 1.5 | 0.2-10.41 |
| Female gender | 22 | 0.3 | 2.7 | 0.3-22.6 |
| <7 years of age | 14 | 0.2 | 3.7 | 0.46-30.8 |
| AFM | 12 | 0.003 | 24.0 | 2.9-197.6 |
Legend: AFM: acute fulminant myocarditis; CI: confidence interval; OR: odds ratio; PCR: polymerase chain reaction.
Dividing patients into three groups according to EF (>55%, 40%-55%, <40%) showed that patients with EF 40-55%were at 20-fold increased risk of developing DCM compared to patients with preserved EF (Table 5).
The follow-up period was 27.14±36.52 months. Patients with AFM who survived significantly improved their EF during the follow-up period (p<0.001).
Sudden cardiac death was more commonly observed in infants (2.7 months of age, IQR -146.2 months; 3/4 patients; p=0.004). Patients with AFM had a higher mortality rate (4/12; p<0.001). Gender did not influence survival (p=0.6). Children with three positive diagnostic criteria had more common fatal outcomes (3/4) than the others (p=0.03). In comparison to patients who survived, patients who died had poorer systolic function at admission (EF 33.0±10.10 vs. 54.8±13.8%, p=0.003; FS 16.5±7.3 vs. 30.7±9.6%, p=0.005).
Intravenous immunoglobulin was administered in 16/62 patients in our study. Seven of those developed DCM and three died. Children with adverse outcomes had lower EF at admission in comparison with children without adverse outcomes (36.0±7.8 vs. 46.8±8.5% p=0.04). During the follow-up period, statistically significant improvement in LVEF in IVIG treated patients were registered (40.3±10.1 vs. 59.8±9.2%, p≥0.001).
DiscussionAn adverse outcome in AM is estimated to occur in 43% of pediatric patients during in-hospital stay and up to 16% in one year follow-up.1 In our study, myocarditis occurred more frequently in boys, which is consistent with some other studies.1,2,6,9 The occurrence of myocarditis had trimodal age-at-onset, although some previous studies demonstrated bimodal age distribution.1,2,6,9 Those with a poor outcome (DCM development) were younger (under the age of seven) and more likely to be female. According to a multicentric analysis conducted at seven university hospitals in Germany, children under the age of two were more likely to have complications, whereas gender did not affect the outcome of the disease.2 A study conducted in the USA concluded that cardiac transplantation was significantly more common in patients <12 years,10 while the authors of the Myocarditis Registry for Children and Adolescents - MYKKE study concluded that the risk of severe disease declines by 14% annually with age.8 Some authors have also found that females with AM had lower EF, underwent heart transplantation more commonly, were readmitted due to HF, and died.2
Butts et al. concluded that it was more frequent for patients with signs and symptoms of respiratory failure and gastrointestinal symptoms to have moderate to severe ventricular dysfunction.2 Our research found that none of the patients with chest pain and pericarditis had this adverse outcome, while patients with signs and symptoms of HF were at increased risk of DCM.
Our study showed that CK, CK-MB, SGOT, SGPT, and LDH values were significantly higher in the group of patients who developed DCM, whereas the difference between the groups was not found comparing cTn levels. Rodriguez-Gonzalez et al. observed that elevated cTn levels did not affect disease outcome.1 Troponin T elevation was reported to have specificity of 86% and sensitivity of 71% in children.3 The study conducted in adults concluded that the sensitivity of elevated cTnI for the entire group was low (34%), but specificity was satisfying (89%).11 Children with AFM had lower CRP values, which stood in contrast to adults.12,13 The cutoff value for LDH is 1780 mmol/l with 80% sensitivity and 100% specificity defined by ROC curve, while other analyzed parameters had lower specificity than LDH. Consequently, LDH could be a meaningful prognostic value for the outcome of pediatric myocarditis. Some other researchers concluded that LDH isoenzyme 1 might be increased in patients with idiopathic myocarditis, and patients with HF and pressure and volume overload had increased level of this enzyme.14
Risk of DCM development rose five-fold in PCR-positive myocarditis. According to the literature data, viral AM induced moderate-severe ventricular dysfunction, and it was the cause of 18% of DCM in childhood.2,5 PCR-positive myocarditis accounted for 32.3% of patients. Although viral PCR testing on EMB samples is a clinically available test, PCR assessment of virus from the respiratory tract and other sites has also been recommended in children.15 A small pilot study showed that PCR in the blood samples at the time of AM was positive in 43% of the patients compared with only 4% of children receiving a same-day surgery elective procedure.15 The majority (89%) of positive viral PCR results were observed in infants. Of all PCR-positive infants, 50% had adverse outcomes (two developed chronic dilated cardiomyopathy, one underwent heart transplantation, and one died).16 In our study group, age was not a differentiating factor between children with PCR-positive and PCR-negative myocarditis, but patients with PCR-positive myocarditis had more common adverse outcomes.
An echocardiogram is still the most useful diagnostic method to verify LV contractility disorder and valve insufficiency, which most commonly occurs during AM.5,7 An echocardiographic assessment of myocardial function showed that patients with systolic impairment were at increased risk of DCM, while EDD Z score >2+ increased the risk of a poor outcome by almost 12-fold. Rodriguez-Gonzalez et al. and researchers from the MYKKE study, established that EF<30% was an independent risk factor for DCM.1,9
Some studies conducted in a pediatric population have shown that 69% of children had spontaneous recovery of myocardial function at one-year follow-up.1 We demonstrated that only 17.7%of patients developed DCM. AFM was an independent risk factor for DCM in AM, but children with EF 40-55% were at the highest risk for DCM. This might be explained due to patients with AFM having predominantly immunological rather than direct viral destruction.8,17–19 Consequently, in patients who survived the acute phase, the long-term outcome seems favorable and better than patients who were presenting with insidious chronic disease.20,21 Additionally, some authors concluded that despite its fulminant presentation, AFM has better short- and long-term outcomes than AM.20,22 We encountered patients who survived and had improved heart function during the follow-up period, similar to Yen's findings..19
In our study, 6.5% of patients died. Sudden cardiac death was observed more commonly in infants. According to the literature, mortality is 7-22%, and it is estimated that myocarditis is the cause of death in 17% of adolescents under the age of 16.1,10 Gender did not influence mortality rate. According to the multi-institutional analysis performed by Klugman et al., age and gender did not influence mortality, but patients with myocarditis who died had a higher disease severity score.4 Fatal outcomes were more commonly observed in patients with three of the diagnostic criteria at admission. Mortality was 33.3% in patients with AFM, which was lower in comparison to some other studies.12,21 Some authors concluded that AFM with severe hemodynamic compromise had early mortality of more than 75% in children, especially during the neonatal period and the first year of life.21,22 According to Matsuura et al., AFM was an independent predictor for death.12
We used IVIG in patients with progressive clinical course and signs of HF, and with AFM, although there is not a consistent recommendation for their use.7 Intravenous immunoglobulin modulates the immune response and lead to an improvement in LVEF. Klugman et al. found that IVIG did not have any impact on mortality when analyzing the same patients with extreme severity illness score.4 According to the systematic review and meta-analysis, children who received IVIG had a significantly higher survival rate than those who did not, but it is still unclear whether the duration of high dose IVIG affects the survival of patients with myocarditis.19 In our study group, children treated with IVIG with adverse events had an average LV systolic function under 40%. A meta-analysis showed that patients receiving IVIG had improved LVEF and mortality or the heart transplantation rate was decreased (at the end of follow-up).23
ConclusionFactors associated with poor outcomes included younger age, female gender, signs and symptoms of HF, PCR-positive myocarditis, and poor perfusion associated with worse ventricular function on echocardiogram. According to multinomial logistic regression, AFM was an independent risk factor for DCM, but patients with EF between 40-55% were at highest risk of DCM. Additionally, LDH due to high specificity and high sensitivity could be a significant prognostic value for the outcome of pediatric myocarditis. Children with AFM who survived had improved systolic function during the follow-up period. Sudden cardiac death was more commonly reported in younger children. Additionally, IVIG treated children with adverse events had to average LVEF <35%.
LimitationsThe major limitations of this study were the collation of data from medical records and its retrospective design. The number of patients is insufficient for the conclusion. Analysis of CMR and EMB did not examine what precludes comprehensive analysis.
Conflicts of interestThe authors have no conflicts of interest to declare.