Portuguese is the sixth most spoken language worldwide, with 244 million speakers, the fifth most commonly used language over the internet, by almost 83 million people, and the third most commonly used language on the social media platforms Facebook and Twitter. Portuguese is the official language of eight countries (Portugal, Brazil, Angola, Mozambique, Guinea-Bissau, Cape Verde, São Tomé and Príncipe, and East Timor). Despite the incorporation of native words, and certain differences in grammar and pronunciation, these countries still share a common language, as well as many important health problems such as cardiovascular disease (CVD).1
Currently, two cardiology journals are published worldwide in the Portuguese language: the Portuguese Journal of Cardiology (Revista Portuguesa de Cardiologia, RPC), and Arquivos Brasileiros de Cardiologia (commonly known as ABC Cardiol). These two journals publish the best papers on cardiology and cardiovascular science in the Portuguese language.
The RPC is the official journal of the Portuguese Society of Cardiology. With more than 35 years of continuous publication, it is now a prestigious international journal with global visibility.2
The histories of the Brazilian Society of Cardiology and ABC Cardiol have been intertwined since the beginning. In 2018 ABC Cardiol completed 70 years of existence. It is an open access publication, home reading for all the 14000 cardiologists and other members of the Brazilian Society of Cardiology, with almost one third of its articles coming from non-Brazilian authors. ABC Cardiol is indexed in the major databases and has the highest impact factor of any journal in the area of cardiology and cardiovascular sciences in Latin America.3
Every year both journals publish dozens of high-quality articles. In 2018, the RPC published a total of 194 papers, including 62 original articles, and ABC Cardiol published a total of 240 papers, of which 96 were original articles. Selecting the ten best original articles (Tables 1 and 2) from each journal is bound to be a difficult endeavor, given their overall high scientific quality. Moreover, in the absence of specific metrics, this selection will inevitably be imperfect and influenced by some degree of subjectivity. Nonetheless, a judging committee composed of highly qualified scientists in the field has produced probably the fairest results for the top ten articles from these journals. Both journals have also published several important review papers, which were beyond the scope of this selection.
The 10 best original articles published in 2018 in the Portuguese Journal of Cardiology.
| Authors | Title and link |
|---|---|
| Timóteo et al.4 | Portuguese Registry of Acute Coronary Syndromes (ProACS): 15 years of a continuous and prospective registry https://www.sciencedirect.com/science/article/pii/S2174204918301983 |
| Monteiro et al.29 | The SAFIRA study: a reflection on the prevalence and treatment patterns of atrial fibrillation and cardiovascular risk factors in 7500 elderly subjects https://www.sciencedirect.com/science/article/pii/S2174204918300849 |
| Pereira et al.7 | Factors influencing patient delay before primary percutaneous coronary intervention in ST-segment elevation myocardial infarction: the Stent for life initiative in Portugal https://www.sciencedirect.com/science/article/pii/S0870255117300811 |
| Menezes et al.15 | Comparative analysis of fractional flow reserve and instantaneous wave-free ratio: results of a five-year registry https://www.sciencedirect.com/science/article/pii/S217420491830134X |
| Cardim et al.42 | The Portuguese Registry of Hypertrophic Cardiomyopathy: overall results https://www.sciencedirect.com/science/article/pii/S0870255117305425 |
| Andrade et al.40 | Knowledge about cardiovascular disease in Portugal https://www.sciencedirect.com/science/article/pii/S0870255117306832 |
| Timóteo et al.23 | What is the role of beta-blockers in a contemporary treatment cohort of patients with acute coronary syndrome? A propensity-score matching analysis https://www.sciencedirect.com/science/article/pii/S217420491830388X |
| Fontes-Carvalho et al.56 | Left atrial deformation analysis by speckle tracking echocardiography to predict exercise capacity after myocardial infarction https://www.sciencedirect.com/science/article/pii/S2174204918303520 |
| Rodrigues et al.38 | Body adiposity is associated with risk of high blood pressure in Portuguese schoolchildren https://www.sciencedirect.com/science/article/pii/S2174204918301259 |
| Pereira-da-Silva et al.bib0410 | Optimizing risk stratification in heart failure and the selection of candidates for heart transplantation https://www.sciencedirect.com/science/article/pii/S0870255117300641 |
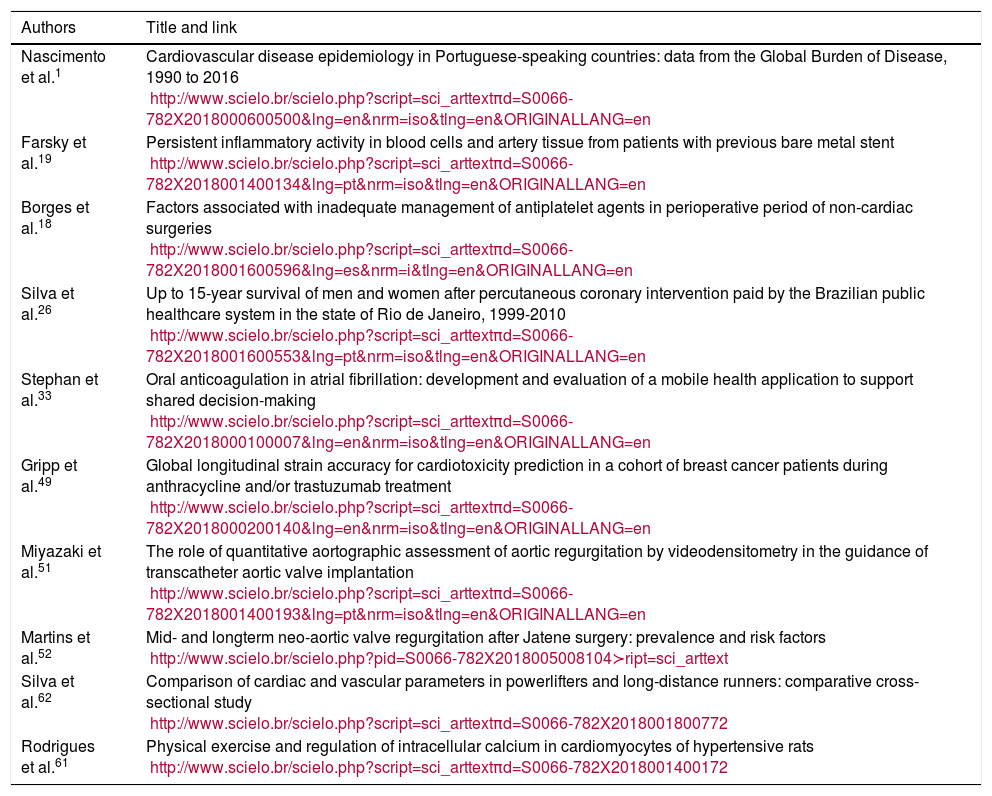
The 10 best original articles published in 2018 in Arquivos Brasileiros de Cardiologia.
| Authors | Title and link |
|---|---|
| Nascimento et al.1 | Cardiovascular disease epidemiology in Portuguese-speaking countries: data from the Global Burden of Disease, 1990 to 2016 http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018000600500&lng=en&nrm=iso&tlng=en&ORIGINALLANG=en |
| Farsky et al.19 | Persistent inflammatory activity in blood cells and artery tissue from patients with previous bare metal stent http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018001400134&lng=pt&nrm=iso&tlng=en&ORIGINALLANG=en |
| Borges et al.18 | Factors associated with inadequate management of antiplatelet agents in perioperative period of non-cardiac surgeries http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018001600596&lng=es&nrm=i&tlng=en&ORIGINALLANG=en |
| Silva et al.26 | Up to 15-year survival of men and women after percutaneous coronary intervention paid by the Brazilian public healthcare system in the state of Rio de Janeiro, 1999-2010 http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018001600553&lng=pt&nrm=iso&tlng=en&ORIGINALLANG=en |
| Stephan et al.33 | Oral anticoagulation in atrial fibrillation: development and evaluation of a mobile health application to support shared decision-making http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018000100007&lng=en&nrm=iso&tlng=en&ORIGINALLANG=en |
| Gripp et al.49 | Global longitudinal strain accuracy for cardiotoxicity prediction in a cohort of breast cancer patients during anthracycline and/or trastuzumab treatment http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018000200140&lng=en&nrm=iso&tlng=en&ORIGINALLANG=en |
| Miyazaki et al.51 | The role of quantitative aortographic assessment of aortic regurgitation by videodensitometry in the guidance of transcatheter aortic valve implantation http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018001400193&lng=pt&nrm=iso&tlng=en&ORIGINALLANG=en |
| Martins et al.52 | Mid- and longterm neo-aortic valve regurgitation after Jatene surgery: prevalence and risk factors http://www.scielo.br/scielo.php?pid=S0066-782X2018005008104≻ript=sci_arttext |
| Silva et al.62 | Comparison of cardiac and vascular parameters in powerlifters and long-distance runners: comparative cross-sectional study http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018001800772 |
| Rodrigues et al.61 | Physical exercise and regulation of intracellular calcium in cardiomyocytes of hypertensive rats http://www.scielo.br/scielo.php?script=sci_arttextπd=S0066-782X2018001400172 |
In 2018, the RPC reported the 15-year results of the Portuguese Registry of Acute Coronary Syndromes (ProACS).4 This is a multicenter continuous and ongoing registry which has already included more than 45000 events from 45 centers. It is one of the largest national registries in this field, only exceeded by the SWEDEHEART5 and MINAP6 registries. The article provides important information on the epidemiology of acute coronary syndrome (ACS) and developments in its treatment. It demonstrates that the clinical profile of ACS patients changed little over the study period, and the proportion of ST-elevation myocardial infarction (STEMI) remained stable (45%). More importantly, over the years, there were major improvements in the overall quality of ACS care. For example, more than 85% of STEMI patients in Portugal now receive reperfusion therapy, mainly by primary percutaneous coronary intervention (PCI) (only 5.2% underwent thrombolysis). This improvement in ACS care led to a marked reduction in in-hospital mortality, which decreased from 6.7% in 2002 to 2.5% in 2016. This is a striking achievement by the cardiovascular community. Nevertheless, the work is not finished, and this study also shows important gaps in ACS care that need to be addressed. Unfortunately, time to reperfusion has not improved sufficiently, and there is an urgent need to improve both patient delay (time from symptom onset to first medical contact) and system delay times.
In another interesting article published in 2018, Pereira et al.7 assessed the determinants of patient delay in the Portuguese health system in 994 patients with suspected STEMI. Although most healthcare systems focus on door-to-balloon time as the main performance measure,8 it is important to understand and address the reasons for patient delay.9 The investigators observed that patient delay was excessive (nearly 120 min) and identified five predictors of greater patient delay:
- 1)
age >75 years;
- 2)
symptom onset between 0:00 and 8:00 a.m.;
- 3)
attending a primary care unit before first medical contact;
- 4)
not calling the national medical emergency number; and
- 5)
self-transport to the emergency department.
This article provides valuable information for planning more effective patient-directed campaigns that can decrease patient delays and improve STEMI management and prognosis.10
The 2018 European guidelines on myocardial revascularization stress the importance of hemodynamic assessment of intermediate-grade coronary artery lesions, which can be done by fractional flow reserve (FFR) or instantaneous wave-free ratio (iFR).11 iFR is a new technique for assessing the severity of coronary stenosis that has the advantage of not requiring the administration of a vasodilator, such as adenosine. Two recently published randomized trials have shown comparable clinical results between these two techniques in patients with intermediate-grade stenosis.12,13 However, some studies have shown that there may be inconsistencies between the two measurements.14 In a provocative article published in the RPC, Menezes et al.15 report their experience directly comparing FFR and iFR information in 150 patients. They demonstrated that, in general, FFR and iFR were concordant, but in a significant proportion of cases (13%) the results differed between the two techniques. This article thus makes an important contribution to the ongoing discussion about the underlying mechanisms responsible for this discordance and their clinical implications.16–18
An issue that remains open in coronary artery disease care is higher mortality after coronary artery bypass grafting (CABG) in patients with previous stent implantation. Farsky et al.19 analyzed gene expression and inflammatory markers (LIGHT, IL-6, ICAM, VCAM, CD40, NF-κB, TNF, TNF-α, IFN-γ) in peripheral blood cells and in coronary artery tissue obtained during CABG in patients with stents (n=41) compared to controls (n=26). They observed that patients with stents showed higher TNF (p=0.03) and lower CD40 gene expression (p=0.01) in peripheral blood cells than controls without stents. In coronary artery samples, TNF protein staining was higher in patients with stents, not only in the intima-media layer (5.16±5.05 vs. 1.90±2.27; p=0.02), but also in adipose tissue (6.69±3.87 vs. 2.27±4.00; p<0.001), in which Il-6 protein staining was also higher (p=0.04). They concluded that higher systemic levels of inflammatory markers in patients with stents may contribute to a worse clinical outcome, improving our understanding of the pathophysiological changes that occur in patients with coronary stents who undergo coronary artery bypass grafting.
Another challenge in coronary artery management is cardiac complications and deaths in the postoperative period following non-cardiac surgery, mainly due to acute myocardial infarction (MI). Antiplatelet agents are the cornerstone for primary and secondary prevention of cardiovascular events. Borges et al.20 conducted a cross-sectional study to assess factors associated with inadequate management of antiplatelet agents in the perioperative period of non-cardiac surgery. Their sample consisted of adult patients undergoing non-cardiac surgery using aspirin or clopidogrel (n=161). Management failed to comply with the recommendations in the guidelines in 80.75% of the sample. Multivariate analysis showed that patients with a higher level of education (odds ratio [OR] 0.24; 95% confidence interval [CI] 0.07-0.78), and those with a previous episode of MI (OR 0.18; 95% CI 0.04-0.95) were more likely to use a therapy complying with the guidelines. These findings emphasize the importance of a heart team to develop a patient-directed educational tool that will improve patients’ adherence to the treatment of coronary artery disease.
In medicine, it is important to keep questioning established dogmas. For decades, the use of beta-blockers has been considered a cornerstone of medical therapy after ACS, with a class I or IIa indication for patients after STEMI and non-STEMI, respectively.19,20 However, in the era of reperfusion therapy, several studies have questioned this indication, especially in patients without left ventricular dysfunction.21,22 In the November issue of the RPC, Timóteo et al.23 published an article on this subject which adds more fuel to the fire in this ongoing discussion. Based on a single-center registry, they used propensity-score analysis to analyze the one-year outcome of patients treated with beta-blockers in a sample of 1520 post-ACS patients. They observed that beta-blocker use was an independent predictor of total mortality, including in patients with normal or mildly reduced ejection fraction. This analysis had some limitations. Although they used propensity-score matching, some caution is advised in the interpretation of these results because of residual confounding. Moreover, compliance with treatment and, more importantly, the reasons for not prescribing a beta-blocker could not be assessed in this study. Nevertheless, the study is important because it highlights the urgent need to design pragmatic clinical trials to reassess the effectiveness and safety of beta-blockers in the modern era of reperfusion therapy.
Also, in medicine, it is important to keep questioning the effectiveness of treatment given to our patients. Silva et al.26 studied the survival rate of adult patients with ischemic heart disease treated with PCI in the state of Rio de Janeiro, from 1999 to 2014, paid by the Brazilian public healthcare system. They presented data on 19263 patients (aged 61±11 years, 63.6% men), and survival rates of men vs. women at 30 days, one year and 15 years were 97.3% (97.0-97.6%) vs. 97.1% (96.6-97.4%), 93.6% (93.2-94.1%) vs. 93.4% (92.8-94.0%), and 55.7% (54.0-57.4%) vs. 58.1% (55.8-60.3%), respectively. They also observed that the oldest age group was associated with lower survival rates in all periods; patients treated by PCI with stent placement had better survival than those without stent placement during a two-year follow-up; and women had better survival than men at 15 years after PCI. These findings in a real-world population may help physicians to make decisions regarding the indication for PCI, considering the benefits and risks observed with this procedure.
ArrhythmiasAtrial fibrillation (AF) is the most common sustained arrhythmia, and a significant risk factor for stroke, heart failure and mortality.25,26 The SAFIRA study,29 recently published in the RPC, aimed to determine the prevalence and epidemiology of AF in a large sample of 7500 elderly Portuguese individuals. The study included a significant subset of 400 individuals who underwent 24-hour Holter monitoring and another subset of 200 subjects who were fitted with an event recorder for two weeks to identify paroxysmal AF. Several interesting findings came from this study. First, the authors observed a very high prevalence of AF in this elderly population (9%), which was higher than previously reported.28,29 Second, more than one-third (35.9%) of AF patients were not aware of having the disease, and 18.6% had paroxysmal AF, which highlights the need for more systematic AF screening.30 More importantly, in this real-world study the rates of anticoagulation were very disappointing. Although the mean CHA2DS2-VASC score was high (3.5±1.2), most AF patients (56.3%) did not receive anticoagulation and only 25.8% were considered to be adequately anticoagulated. This study thus highlights the enormous challenges in the diagnosis and management of AF in elderly patients and the urgent need to implement specific healthcare policies (involving patients, caregivers, physicians and health authorities) that can tackle these important problems.
As stated above, the treatment of atrial fibrillation is a challenge in clinical practice, especially with regard to the use of oral anticoagulants, which are fundamental to the prevention of stroke. Considering the challenges associated with this therapy, Stephan et al.31 hypothesized that mobile health support for shared decision-making may improve patients’ knowledge and optimize the decision-making process. The authors developed an app (App aFib) to be used during clinical visits, including a video about atrial fibrillation, risk calculators, explanatory graphics and information on the drugs available for treatment. In the pilot phase, 30 patients interacted with the app, which was evaluated qualitatively, and through a disease knowledge questionnaire and a decisional conflict scale. The number of correct answers in the questionnaire about the disease was significantly higher after the interaction with the app (from 4.7±1.8 to 7.2±1.0, p<0.001), and the average score on the decisional conflict scale, administered after selecting the therapy with the support of the app, was 11±16/100 points, indicating a low decisional conflict. Although these were initial findings, App aFib improves patients’ disease knowledge, and in the future more studies may determine whether this finding can be translated into clinical benefit.
Cardiovascular disease prevention and epidemiologyThe presence of cardiovascular risk factors in childhood creates a lifelong burden which increases the risk of cardiovascular disease in adulthood.32,33 Several studies have shown the importance of assessing risk factors and promoting healthy lifestyles throughout the lifespan, starting as early as in preschool children.34,35 In an interesting study published in 2018, Melo Rodrigues et al.36 analyzed the prevalence and interrelation of cardiovascular risk factors in a sample of 1555 schoolchildren (6-9 years). They found a very high prevalence (29.1%) of overweight and obesity in this population, which demonstrates the magnitude of the childhood obesity epidemic.37 The prevalence of high-normal blood pressure (4.5%) and hypertension (3.7%) was also much higher than expected. There was a strong association between anthropometric body fat indicators and blood pressure, which highlights the need for blood pressure measurement in obese children. However, the most important take-home message from this study is that the lifestyle behaviors of adults are linked to their previous exposures during childhood,31 and so cardiovascular health promotion should involve all ages, starting with preschool children, and the entire family.38
It is also known that lifestyle behaviors associated with increased risk of cardiovascular disease are influenced by the individual's health-related knowledge (health literacy) and by their perception of the risk of disease.39 Improving health literacy should thus be viewed as an essential tool to reduce the global burden of cardiovascular disease and to improve risk factor control. In an innovative article published in 2018 in the RPC, Andrade et al.40 assessed specific knowledge on cardiovascular disease and its relationship with sociodemographic factors, health literacy and clinical history, in a large sample of 1624 Portuguese individuals. The results showed a striking deficit in cardiovascular health-related knowledge, with only around one-third of the population being able to estimate their risk of myocardial infarction or stroke. Interestingly, participants identified non-smoking and a healthy diet as the main behaviors for cardiovascular disease prevention, and attributed lower importance to blood pressure control. It was also observed that only a very low percentage of individuals would call the national emergency number in the presence of symptoms suggestive of a possible stroke or myocardial infarction, as also demonstrated in other studies.41 This study clearly shows that there are important gaps in cardiovascular health-related knowledge in the general population. All those involved – physicians, the medical community, and society in general – need greater awareness of the importance of improving health literacy in the community. This is a new and important strategy to help prevent cardiovascular disease.
It is essential to be aware of gaps in cardiovascular healthcare, and knowledge of the common problems and solutions shared by Portuguese-speaking countries (PSC) can provide useful data regarding the similarities and differences between them, especially concerning actions that are successful in combating CVD. Nascimento et al.1 described trends in CVD-related morbidity and mortality in the PSC between 1990 and 2016, stratified by gender, and their association with the respective sociodemographic indices using the 2016 Global Burden of Disease data and methodology. They observed large differences, mainly related to socioeconomic conditions, in the relative impact of CVD burden in the PSC. Among cardiovascular diseases, ischemic heart disease was the leading cause of death in all the PSC in 2016 except for Mozambique and São Tomé and Príncipe, where it was exceeded by cerebrovascular disease. The most important attributable risk factors for CVD in all the PSC are hypertension and dietary factors. Genetic factors, related to the common cultural identity of the PSC, and host-specific factors, as well as the considerable social inequalities within these countries, may have contributed to the mortality rates observed. Collaboration between the PSC could allow successful experiences in combating CVD to be shared between these countries.
Cardiomyopathies and valvular heart diseaseIn the January 2018 issue of the RPC, Cardim et al.42 reported the overall results of the Portuguese Registry of Hypertrophic Cardiomyopathy (PRo-HCM), which included 1042 patients from 29 centers. This is one the largest and most significant HCM registries worldwide, and provides a detailed contemporary assessment of the clinical profile, management strategies and outcomes of HCM in Portugal. Among the main conclusions was that age at diagnosis of HCM is relatively advanced, with more than one fourth of patients diagnosed over the age of 65 years. The use of cardiac magnetic resonance imaging for HCM assessment was limited, but more than 50% of patients underwent genetic testing. Long-term mortality (0.65%/year) and the risk of sudden cardiac death (0.22%/year) were low, but morbidity remained considerable. This registry shows that there are important differences between the guidelines and clinical practice in HCM management, which has also been demonstrated in other registries.43,44 This may be the result of differences in the clinical course of HCM representing the heterogeneous spectrum of the disease. Finally, these data highlight the importance of clinical registries as a source of information that should be used to inform practice and also to influence the writing of the guidelines.45
Advances in non-invasive cardiac imaging have provided important new insights into the pathophysiology of valvular heart disease and cardiomyopathies, and the diagnosis of implanted device- or bioprosthesis-related complications.46 Gripp et al.47 used global longitudinal strain to assess the incidence of cardiotoxicity in 49 patients treated for breast cancer, and the independent factors associated with it. Cardiotoxicity was identified in five patients (10%), at the third (n=2) and sixth (n=3) month of follow-up. Strain was independently associated with the event (p=0.004; hazard ratio 2.77; 95% CI: 1.39-5.54), with a cutoff point of an absolute value of -16.6 (area under the curve [AUC] 0.95; 95% CI: 0.87-1.0) or a percentage reduction of 14% (AUC 0.97; 95% CI: 0.9-1.0). The authors concluded that a 14% reduction in strain (absolute value of -16.6) enabled early identification of patients who might develop anthracycline and/or trastuzumab-induced cardiotoxicity.
The added diagnostic and prognostic value of combining imaging techniques (fusion imaging) is increasingly recognized. The Valve Academic Research Consortium-2 consensus document recommends quantitative and semi-quantitative hemodynamic assessment of aortic regurgitation (AR) severity by echocardiography,48 and moderate-to-severe AR is defined as valve failure that is associated with poor outcome and mortality. Miyazaki et al.49 investigated a quantitative angiographic assessment of AR by videodensitometry before and after balloon post-dilatation (BPD), since this technique provides an accurate assessment of the severity of paravalvular leak and correlates with increased mortality and impaired reverse cardiac remodeling by echocardiography after transcatheter aortic valve implantation (TAVI). The authors showed that videodensitometry AR (VD-AR) decreased significantly from 24.0% [18.0-30.5] to 12.0% [5.5-19.0], and the relative delta of VD-AR after BPD ranged from -100% (improvement) to +40% (deterioration). Significant AR (VD-AR >17%) was observed in 47 patients (77%) before, and in 19 patients (31%) after BPD. They concluded that VD-AR after TAVI provides a quantitative assessment of post-procedural regurgitation and can help in deciding whether BPD should be performed and in determining its efficacy.
The increasing number of children with evolving congenital heart diseases, due to reductions in associated mortality, especially in recent years, means that the physicians and institutions that deal with them must be better prepared. Jatene surgery has become the surgical procedure of choice to repair transposition of the great arteries (TGA) in neonates and infants, but the behavior of the neo-aortic valve is currently a cause of concern because of the potential need for late reoperation. Martins et al.52 assessed the prevalence and risk factors of neo-aortic valve regurgitation in 127 patients in the late postoperative period. The incidence of mild regurgitation was 29% and of moderate regurgitation was 18%, in a long follow-up. These patients had a higher aortic annulus Z-score, although the reoperation rate due to neo-aortic regurgitation associated with aortic dilatation was only 1.5%, all in patients with complex TGA. This study shows that, although the incidence of reoperation after Jatene surgery is low, these patients require close vigilance, since neo-aortic valve regurgitation is a time-dependent phenomenon. Another finding was that one of the major risk factors for neo-aortic valve regurgitation was preoperative pulmonary artery diameter.
Cardiac function, exercise capacity and heart failureSeveral studies have shown that left atrial (LA) size and function are important predictors of cardiovascular events in several clinical settings and may be involved in the progression to heart failure.51,52 In another interesting article published in the RPC, Fontes-Carvalho et al.53 analyzed the role of different indices of LA function assessed by speckle tracking echocardiography as determinants of exercise capacity by cardiopulmonary exercise testing (CPET) in 94 patients after MI. They found a significant correlation between exercise capacity and LA conduit function, but not with contractile function. LA longitudinal strain was also associated with worse exercise capacity parameters, suggesting that this echocardiographic parameter can be used to predict reduced exercise capacity. Finally, it was shown that LA functional parameters were interdependent with LV diastolic function, highlighting the pathophysiological importance of correct atrioventricular coupling. This study demonstrates that although the left atrium has often been considered a bystander in the regulation of cardiac function, the availability of new echocardiographic parameters (such as those derived from speckle tracking) shows the clinical utility of LA assessment as an important functional and prognostic marker in various clinical settings, especially heart failure (HF).54
HF patients are at significant risk of cardiovascular events. Various studies have tried to improve risk stratification tools to predict HF hospitalizations or the need for heart transplantation. The most commonly used score is the Seattle Heart Failure Model, which is based on 24 clinical variables.55 Other scores are also available,56 but there is an ongoing need to improve risk stratification in HF. In the February issue of the RPC, Pereira-da-Silva et al. demonstrate that VE/VCO2 slope, obtained from CPET, can be a good predictor of events in patients with HF with reduced ejection fraction (<40%). Although most previous studies have assessed the role of peak VO2 as a prognostic marker, the VE/VCO2 slope is a particularly interesting parameter, because it reflects ventilatory efficiency and is independent of the level of patient effort.57 The authors identified a threshold VE/VCO2 slope of >39 as an excellent marker of worse outcome, with a c-statistic of 0.79. Nevertheless, it has been said that there are no magic numbers in medicine. This is especially true in the selection of HF patients for heart transplantation, for which individual clinical decisions require a team-based approach, extensive clinical experience, and a multiparametric approach. This interesting study highlights the importance of integrating information provided by CPET, especially on VE/VCO2, as another important clinical parameter to better stratify these patients.
Exercise training induces cardiovascular adaptations secondary to changes in blood pressure, as well as other hemodynamic and metabolic changes in response to physical exertion that are in most cases seen as beneficial by cardiologists. Rodrigues et al.58 assessed the effects of aerobic exercise training on contractility and intracellular calcium (Ca2+) transients in cardiomyocytes, and on the expression of microRNA-214 (miR-214) in the left ventricle of spontaneously hypertensive rats. They demonstrated that exercise training reduced systolic blood pressure and increased the availability of intracellular Ca2+ by accelerating the sequestration of these ions in the left ventricular myocytes of hypertensive rats, despite increased expression of miR-214 and maintenance of cell contractility. This study confirmed the antihypertensive effects of aerobic exercise, as reported previously.
But can any level of exercise be beneficial to everyone? Silva et al.59 hypothesized that athletes engaging in high-intensity strength training for long periods show changes in cardiac structure associated with reduced cardiac function compared to long-distance runners, and long-term exposure to high-intensity strength training could lead to a reduction in endothelial function caused by pressure overload. They assessed 40 high-performance athletes (powerlifters, n=16; runners, n=24) and assessed heart structure and function by echocardiography and measuring systolic and diastolic blood pressure, flow-mediated dilation, peripheral vascular resistance (PVR), maximum force (squat, bench press, and deadlift), and maximal oxygen uptake by spirometry. The authors concluded that cardiovascular adaptations are dependent on training modality, and associated borderline structural cardiac changes are not accompanied by impaired function in powerlifters. However, a mild increase in blood pressure seems to be related to PVR rather than to endothelial function.
ConclusionsWe hope this review of the best in cardiology and cardiovascular science published last year in the Portuguese language by two major journals can help our readers update their knowledge in an easy and pleasant format and at the same time stimulate them to go deeper into the articles in their field of expertise. The specific areas covered by this review include coronary artery disease, arrhythmias, cardiovascular disease prevention and epidemiology, cardiomyopathies and valvular heart disease, and cardiac function, exercise and HF. Articles published in all these fields presented important innovations, new and original information with direct effect on routine clinical patient management, and new insights into and better understanding of disease processes and treatment. Population and epidemiological data of particular importance for Portuguese-speaking countries were also presented.
Conflicts of interestThe authors have no conflicts of interest to declare.
Please cite this article as: Fontes-Carvalho R, Oliveira GM, Gonçalves L, Rochitte CE. O ano de 2018 em Cardiologia: Uma visão geral da ABC Cardiol e RPC. Rev Port Cardiol. 2019. https://doi.org/10.1016/j.repc.2019.01.004